Animal Ethics Concerns Could Be More Pronounced in Islet Xenotransplantation
Main Article Content
Abstract
Photo by Towfiqu barbhuiya on Unsplash
Abstract
Type 1 diabetes mellitus (T1D) necessitates life-sustaining insulin therapy or islet allotransplantation, which is limited by organ scarcity. While islet xenotransplantation offers a solution to donor shortages, patient perceptions regarding this emerging therapy remain unexplored. This small-scale study tested what would happen to patient support for xenotransplantation when T1D patients learned that upwards of 50 pigs may be needed to treat one adult human patient. Patient viewpoints toward islet xenotransplantation are important to incorporate into xenotransplantation research, as they may impact future clinical uptake. While our sample size is limited, we cautiously suggest that animal ethics concerns regarding xenotransplantation may extend to the magnitude of animals required to treat a single patient. As clinical trials advance, addressing these specific patient-centered values and risk tolerances is essential for developing informed consent frameworks and therapies that are sensitive to patient concerns.
Introduction
Type 1 diabetes mellitus (T1D) is a chronic autoimmune disease characterized by immune-mediated destruction of pancreatic beta cells, resulting in absolute insulin deficiency. It affects over 8 million people globally, of whom 20 percent are under 20 years old.[1] Despite advances in treatment, many patients face challenges related to insulin dependence, including risks of severe hypoglycemia and complications stemming from poor glycemic control. Treatment options for T1D also remain limited. Islet allotransplantation, an alternative treatment for T1D, remains limited by the scarcity of donor organs, the need for lifelong immunosuppression, and the decline in graft survival over time. Pancreatic beta cell islet xenotransplantation (genetically modified porcine-to-human transplantation) is an alternative to exogenous insulin therapy.[2] Researchers estimate it would take between 25-50 piglets to provide enough islets to treat one adult human.[3] This ratio of 25:1 or 50:1 is much different from the ratio in solid organ xenotransplantation, which is often framed as one pig to one or multiple patients.
Understanding how accepting the public and, more importantly, patients, are toward xenotransplantation is a critical component of it being accepted as a clinical alternative to exogenous insulin therapy or allotransplantation. Several studies have examined attitudes toward xenotransplantation, but most focus on solid organ transplantation rather than on islet xenotransplantation.[4]
This study explores a research question that, to our knowledge, has never been tested empirically: Would learning that 25-50 piglets may be required to treat one adult change T1D patients’ attitudes toward islet xenotransplantation?
Methods
We conducted a cross‐sectional pilot study from June to December 2025. We gave our survey to patients with T1D who were part of a diabetes support group in New Jersey. The research team developed the survey in Qualtrics (Provo, Utah) in consultation with experts in endocrinology, bioethics, and quantitative methods, and the survey was informed by prior xenotransplantation studies conducted by the principal investigator and by a review of the literature.[5] The initial draft of the survey was pilot-tested among a small sample at the research team’s university and then revised as needed for clarity.
After ethics approval was obtained,[6] participants were recruited via two methods: in-person at insulin user support groups and through posting on the online social media support group. Participants were 18 years of age or older with a self-reported diagnosis of T1D. The electronic survey contained an informed consent form that asked for an acknowledgement before the participant was allowed to proceed with the survey. Qualtrics collected the data. Because of the small sample size, the research team used descriptive statistics (counts, percentages) to analyze attitudes.
Results
Nineteen complete responses were collected. Twenty participants began the survey; one stopped after the demographic section, resulting in a 95 percent completion rate. Due to the nature of participant recruitment, overall response rate was unable to be calculated as we were unable to determine how many potential participants viewed the survey flyer in the online support group. Demographic characteristics of participants can be viewed in Table 1. Eighteen of the nineteen participants relied on insulin injections daily to control their T1D.
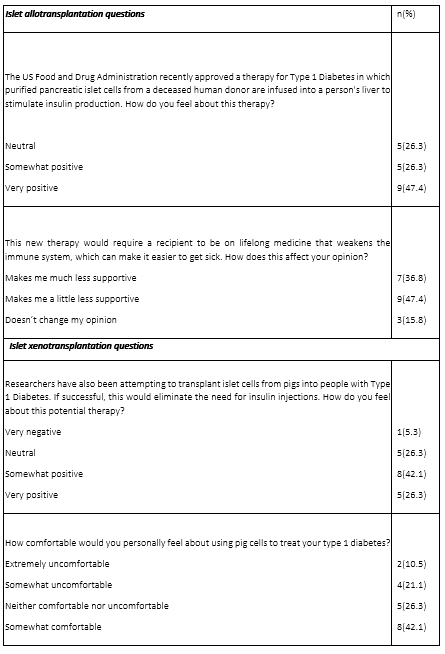
Participants were informed about two emerging therapies–islet allotransplantation and islet xenotransplantation–and asked a series of questions about each of these (Table 2). Islet xenotransplantation is the focus here. Participants were told that researchers have been attempting to transplant islet cells from pigs into people with T1D, which could eliminate the need for insulin injections if effective, and asked how they felt about it. When given response choices ranging from very positive to very negative, initially, five participants (26 percent) checked off “very positive”; eight participants (42 percent) “somewhat positive”; only one participant (5 percent) responded “very negative,”; and five participants (26 percent) were neutral. When participants were asked how comfortable they personally would be if clinicians used pig islets to treat their T1D, six participants (32 percent) stated they were either “extremely uncomfortable” or “somewhat uncomfortable,” while five participants (26 percent) were neutral and eight (42 percent) stated they were “somewhat comfortable.”
Participants were then informed that it may take 25 or more piglet donors to treat one adult human with T1D and asked how they felt about that. The survey provided three options. Five participants (26 percent) responded that this would make them “much less willing to support this research,” and six participants (32 percent) responded that this would make them “somewhat less willing to support this research.” Eight participants (42 percent) responded that their view remained the same with the new information.
Discussion
When informed that treating a single adult might require islet cells from 25 or more piglets, over half of the participants (58 percent; 11/19) reported that this made them less willing to support the research. While we recognize the limitations inherent in a small-scale study, the findings cautiously suggest that patient objections to xenotransplantation grounded in animal ethics issues may extend beyond the mere use of animals to include concerns about the number of animals required. Ethically, this raises questions of proportionality—whether the therapeutic benefit to one human justifies the use of dozens of animal lives. For some patients, the 25:1 ratio may cross an ethical threshold. The survey question that revealed the need to use 25 or more animals for one person’s treatment asked whether the participants would change their view, but the response options used language about “supporting research”. The survey did not ask whether they would be willing to accept the therapy personally knowing 25 or more animals were necessary to treat one person. It is possible that the discomfort or negative view toward such research would be even more pronounced if people had to consider their own care, or alternatively, that when faced with a possible solution for themselves, participants may waver on their discomfort level and compromise their animal ethics position.
Limitations
The interpretation of these findings is constrained by the limitations of a small-scale study. With a small sample size (n=19), our results are descriptive and cannot be generalized to the broader T1D population. Furthermore, the sample was demographically homogenous, consisting primarily of white, female, and highly educated participants. As perceptions of medical trust, animal welfare, and risk tolerance vary significantly across cultural and socioeconomic lines, future studies must recruit a more diverse cohort to ensure that consent frameworks are inclusive and equitable.
Conclusion
This study provides preliminary insight into the complex attitudes of individuals with T1D toward islet xenotransplantation and will inform larger planned studies. The findings demonstrate that patient support for islet xenotransplantation may be fragile. In our sample, the ethical implications of the high donor pig-to-recipient ratio appeared to be a significant barrier to acceptance. As islet xenotransplantation moves from the laboratory to the clinic, biological success cannot be the sole measure of progress. Patient values must inform trial design and be evaluated within the specific context in which trials are conducted. Future research requires larger and more diverse cohorts to determine whether these findings hold in broader populations.
-
Table 1: Demographic information of participants
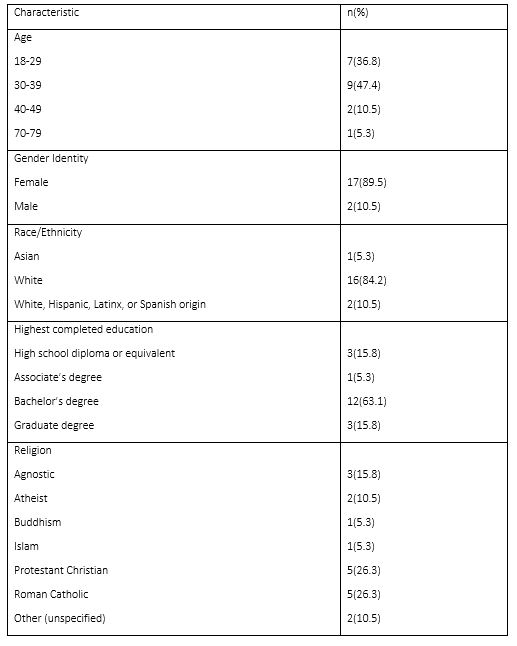
Table 2: Attitudes toward islet allotransplantation and xenotransplantation
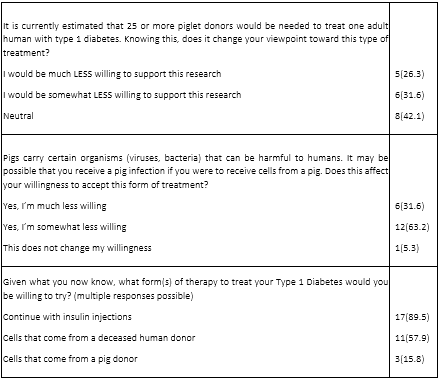
-
[1]Gregory GA, Robinson TIG, Linklater SE, et al. Global incidence, prevalence, and mortality of type 1 diabetes in 2021 with projection to 2040: a modelling study. Lancet Diabetes Endocrinol. Oct 2022;10(10):741-760. doi:10.1016/s2213-8587(22)00218-2
[2] Groth CG, Korsgren O, Tibell A, et al. Transplantation of porcine fetal pancreas to diabetic patients. Lancet. 1994;344(8934):1402-1404. doi:10.1016/s0140-6736(94)90570-3
[3] Ekser B, Bottino R, Cooper DKC. Clinical Islet Xenotransplantation: A Step Forward. EBioMedicine. 2016;12:22-23. doi:10.1016/j.ebiom.2016.09.023; Cooper DKC, Mou L, Bottino R. A brief review of the current status of pig islet xenotransplantation. Front Immunol. 2024;15:1366530. doi:10.3389/fimmu.2024.1366530
[4] Hurst DJ, Rodger D, Padilla LA, Ovalle F. Attitudes toward pig islet xenotransplantation for type 1 diabetes: a scoping review. J Endocrinol Invest. 2025;48(10):2249-2260. doi:10.1007/s40618-025-02626-0; Padilla LA, Hurst DJ, Zink A, Parent B, Kimberly LL. Public attitudes to xenotransplantation: A national survey in the United States. Am J Transplant. 2024;24(11):2066-2079. doi:10.1016/j.ajt.2024.07.018; Al-Haboubi M, Boadu P, Pacho A, Cronin AJ, Mays N. Public views on xenotransplantation from the first representative sample survey in the UK. Lancet. 2025;406(10508):1083-1085. doi:10.1016/S0140-6736(25)01195-X
[5] Padilla et al., 2024; Hurst et al., 2025
[6] There was an anonymous peer review process. The study was approved by the Virtua Health Group IRB #G25061
Article Details

This work is licensed under a Creative Commons Attribution 4.0 International License.